Abstract
Introduction: Somatic calreticulin (CALR) mutations were discovered in patients with essential thrombocythemia (ET) and primary myelofibrosis (PMF) and have been shown to be mutually exclusive with Janus kinase 2 (JAK2) and thrombopoietin receptor (MPL) mutations. Recent studies demonstrated that the binding of CALR mutant proteins to MPL induces constitutive activation of the JAK/STAT pathway, thus causing cellular transformation and abnormal megakaryopoiesis. Additionally, it has been reported that patients carrying homozygously mutated CALR ins5 exhibit myeloperoxidase (MPO) deficiency as a result of the absence of CALR chaperone function. However, the impact of CALR mutant homozygosity vs. heterozygosity in CALR del52 mutations as well as on hematopoietic differentiation has not yet been studied. Furthermore, clonal heterogeneity of hematopoietic stem/progenitor cell (HSPC) populations in a patient, together with technical limitations isolating single clones, are major challenges, when determining the impact of CALR mutant zygosity on clonal composition and diversity in MPN. To overcome these limitations, we generated patient-specific iPS cells carrying homozygous or heterozygous CALR mutations or their wild-type counterparts to study their roles in hematopoietic differentiation.
Methods: iPS cells were generated by reprogramming peripheral blood-derived mononuclear cells from three patients carrying CALR del52, ins5, or del31 mutations using a CytoTune iPS 2.0 Sendai Reprogramming Kit. Individual colonies were picked and screened for CALR genotypes by PCR. Pluripotency of iPS cells was confirmed by immunofluorescences, and the clones were screened for additional mutations using panel-based next generation sequencing (NGS). Subsequently, CALR iPS cells were subjected to embryonic body formation, mesoderm commitment, and hematopoietic differentiation using our standard in vitro differentiation protocol. CD34+ HSPCs were MACS-sorted and characterized by flow cytometry, cytospins and RNA expression analysis on days 10, 15, and 20 during differentiation. Hematopoietic progenitors, erythrocytes, granulocytes, and megakaryocytes were identified by defined lineage markers. MPO expression was assessed by flow cytometry and cytochemical staining.
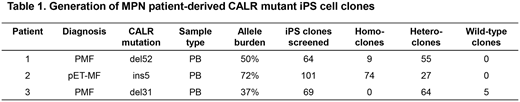
Results: We established patient-specific iPS cells carrying CALR del52, ins5 or del31 mutation after written informed consent (Table 1). Pluripotency markers OCT4, Tra-1-60 and Tra-1-81 expression were confirmed in all iPS cell clones. In accordance with findings in peripheral blood cells, we detected MPO deficiency in homozygous iPS cell-derived CD15+ cells from CALRins5- and, in addition, also from CALRdel52-mutated patients (pMFI=0.0106 and pMFI=0.0187, resp.). Intriguingly, in vitro hematopoietic differentiation assays revealed additional abnormalities, such as decreased CD66b+ granulocytes derived from homozygous CALR del52 or ins5 iPS cells vs. heterozygous iPS cells on day 10 (pdel52=0.0303 and pins5=0.0253, resp.) and a trend towards increased KIThigh+CD45+ cells. Megakaryopoiesis, defined by CD41+CD42b+ cells, was increased in CALRins5 homozygous vs. heterozygous clones (p=0.0031). However, this bias was not observed in all clones, indicating clone-specific megakaryocytic differentiation potential. No phenotypic differences during hematopoietic differentiation were observed in iPS cell-derived progenitors carrying heterozygous CALRdel31 mutation and its isogenic unmutated CALR controls. Furthermore, our NGS data revealed patient-specific sets of co-occurring mutations in iPS cell clones, which may have contributed to the observed patient-specific phenotypes. As an example, the IDH2 R140Q mutation, reported to block cell differentiation, was found in approximately half of the CALRdel52 iPS clones, and these clones failed to differentiate into the hematopoietic lineage in vitro.
Conclusions: We successfully generated patient-specific CALR mutant iPS cells. Upon in vitro differentiation, we detected MPO deficiency and aberrant granulocytic differentiation in CALR homozygous but not heterozygous or wild-type clones. Thus, it is now possible at the single stem cell level to further analyze the molecular mechanisms of CALR-mutant induced MPO deficiency and altered hematopoietic differentiation, in order to better understand disease biology in ET and PMF.
Brümmendorf:Merck: Consultancy; Novartis: Consultancy, Research Funding; Pfizer: Consultancy, Research Funding; Janssen: Consultancy; Takeda: Consultancy.
Author notes
Asterisk with author names denotes non-ASH members.